Stress Urinary Incontinence
Stress urinary incontinence (SUI) is the involuntary leakage of urine that occurs while a person is being physically active or feels pressure in the abdominal area. Uncontrollable urine leakage may happen while exercising, laughing, coughing, or sneezing. It is a form of urinary incontinence that affects one in three women.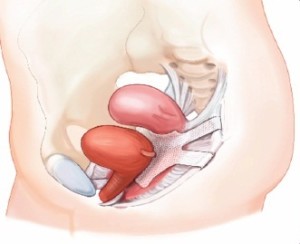
Transvaginal mesh has been used as a treatment option for women suffering from this condition, but medical mesh devices have been subjected to intense scrutiny by the FDA after scientific studies and adverse event reports revealed that they are associated with serious side effects.
Causes of SUI
A diagnosis of stress urinary incontinence stems from a weakening of the sphincter and pelvic floor muscles. If the sphincter isn’t able to stay closed when pressure is applied to the abdomen, urine leaks from the bladder and exits the body.
Causes of stress urinary incontinence include:
- Giving birth multiple times via vaginal deliveries
- Bladder infection
- Hysterectomy
- Nerve damage to back or pelvic area
- Ingesting certain medications
- Obesity
- Smoking
- Chronic cough
- Menopause
The condition is more common among older women because the pelvic muscles get weaker as women age. The extent of the condition varies for each person and can range from mild to severe. It’s possible for men to have stress urinary incontinence as well, but the vast majority of people diagnosed with the condition are women.
Women often seek treatment for this condition because it can diminish their quality of life and cause them to experience extreme discomfort under certain circumstances. The involuntary urine leakage may occur while a woman is at work, attending a social event, performing normal day-to-day activities, or during sexual intercourse. Surgical and non-surgical treatment options that strengthen the pelvic floor muscles and increase bladder support are able to eliminate or reduce the severity of the condition.
Symptoms of SUI
Experiencing the uncontrollable release of urine is the main symptom of stress urinary incontinence. Urine leakage may be minor and only occur sporadically for some women. There are also times when a moderate or heavy amount of urine is released and it dampens a woman’s clothes. Often, the release of urine happens while laughing, exercising, sneezing, coughing, participating in a physical activity, or if the person feels the urge to urinate, but isn’t able to get to a toilet in time.
A physician can properly diagnose the condition by performing a pelvic exam and abdominal ultrasound. Additional tests that measure the flow and pressure of the urine and the patient’s ability to control the urine discharge may also be administered by a healthcare professional. By conducting a series of tests and exams, the physician can also find out if the condition is a symptom of another underlying medical issue.
Treatment with vaginal mesh
Vaginal mesh is a medical device used to repair damaged tissue, support the urethra, and reinforce weakened vaginal walls. The device can be used to treat stress urinary incontinence and pelvic organ prolapse – a medical condition in which organs around the woman’s pelvis don’t remain in place and fall through the vaginal opening due to weakened pelvic floor muscles. A vaginal mesh is comprised of a synthetic material, animal tissues, or a combination of both.
For patients with stress urinary incontinence, the vaginal mesh provides support to the urethra so that urine isn’t released involuntarily. The device is either placed on the lower abdomen or within creases in the groin. An incision is made into the lower abdomen or groin in order to properly place the vaginal mesh device. Usually, patients are able to go home on the same day as the surgery and are able to resume their normal activities within a short period of time.
Side effects linked to vaginal mesh
Some women reported serious transvaginal mesh complications within two years after getting the implants. Some of the manufacturers were not required to conduct clinical safety trials prior to receiving FDA clearance, since the products were considered significantly similar to other medical devices in the market.
According to the FDA adverse event reports and medical studies, serious side effects associated with vaginal mesh are:
- Vaginal mesh erosion
- Vaginal perforation
- Bleeding
- Chronic pain
- Vaginal scarring
- Infections
- Pain during sexual intercourse
- Recurrence of stress urinary incontinence
- Recurrence of pelvic organ prolapse
- Perforation of bladder, bowel, and other nearby organs
The serious injuries require extensive medical treatment, including revision surgery. Attempting to remove the vaginal mesh is difficult and painful if it has become enmeshed in the soft tissues and perforated the organs. Complications during revision surgery may lead to further organ damage, infections, vaginal scarring, and permanent injuries. In some instances, the physicians had to perform multiple surgeries in order to completely remove the medical device and adequately treat patients’ injuries.
Alternative treatment options
Due to the health risks associated with vaginal mesh, some physicians and patients may choose to utilize other methods for treating SUI. The most effective treatment for each patient depends on the severity of the condition and other factors related to the patient’s medical status.
The variety of treatment options available for SUI include:
- Kegel exercises or pelvic floor exercises: exercises that strengthen the pelvic floor muscles and reduce involuntary urine leakage
- Pessary: a device inserted into the vagina by a physician to support the urethra
- Diet and exercise for obese patients in order to reduce pressure on the abdomen
- Prescription medications that help to control the bladder and strengthen the urethra
- Urethral insert: disposable device inserted into the urethra before starting a particular activity that may cause leakage and removed before urinating
FDA warnings and recommendations
The FDA initially approved vaginal mesh as a treatment for stress urinary incontinence in 1996. More than 1,000 adverse event reports were submitted to the FDA after women started receiving vaginal mesh implants. In 2008, the FDA issued a public statement to advise people that the side effects associated with vaginal mesh are serious. Based on the scientific studies and literature analyzed by the FDA, the vaginal mesh wasn’t more effective at treating pelvic organ prolapse or improving the quality of life for patients than traditional non-surgical methods.
On July 13, 2011, the FDA informed the public that using vaginal mesh may pose a greater danger to patients than other treatment options. The FDA also stated that serious complications sustained by patients who received the vaginal mesh were not rare occurrences. Physicians were advised to take this information into consideration when deciding the most suitable treatment option for their patients.
In 2012, the FDA ordered transvaginal mesh manufacturers to conduct studies to assess the efficacy and safety of their medical devices.
Resources
- FDA, Stress Urinary Incontinence (SUI): What is Stress Urinary Incontinence? http://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/ImplantsandProsthetics/UroGynSurgicalMesh/ucm284109.htm
- NetDoctor, Stress Urinary Incontinence (SUI): Facts about SUI and Urinary Incontinence http://www.netdoctor.co.uk/womenshealth/sui/index.shtml
- National Institutes of Health, The Definition, Prevalence, and Risk Factors for Stress Urinary Incontinence, http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1472862/
- Urology Health, Frequently Asked Questions about Stress Urinary Incontinence, http://www.urologyhealth.org/SUI/_documents/_pdf/AUAF_SUI_FAQs.pdf
- FDA Safety Communication: Update on Serious Complications Associated with Transvaginal Placement of Surgical Mesh in Repair of Pelvic Organ Prolapse, http://www.fda.gov/MedicalDevices/Safety/AlertsandNotices/ucm262435.htm
- Europe PubMed Central, Transobturator urethral suspension: mini-invasive procedure in the treatment of stress urinary incontinence in women, http://europepmc.org/abstract/MED/11859672/reload=0;jsessionid=SI6M7hCQ4oIwsb1TRVl0.40

